|
 |
- Search
Abstract
Spontaneous cervical SDH with no underlying pathology is a very unusual condition. To the best of the authors' knowledge, only two cases have been previously reported. A 48-year-old female patient was admitted to our emergency room due to severe neck pain following standing up position with rapid onset of hemiparesis. MRI revealed a dorsolateral subdural hematoma from C3-C5 with cord compression. An emergency laminectomy was planned, but motor weakness gradually improved during surgical preparation. The patient showed substantial clinical improvement and complete recovery was confirmed after 7 days of conservative management without surgical treatment. To determine a differential diagnosis distinct from other conditions such as cervical epidural hematoma, a lumbar spinal puncture was performed. Follow-up MRI performed 10 days after admission revealed complete resolution of the hematoma. We report an extremely rare case of spontaneous cervical spinal subdural hematoma (SDH), present a review of relevant literature, and discuss the etiology, pathogenesis, and prognosis of this case.
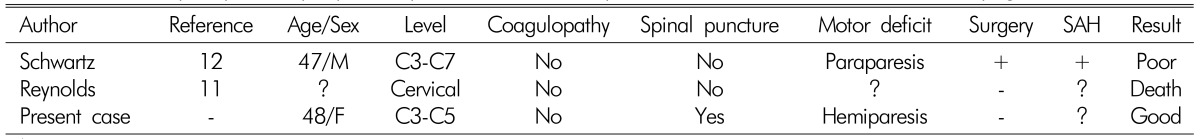
Spinal subdural hematoma (SDH) is a rare clinical entity that frequently occurs in the thoracic regions of the spine. This condition can be caused by major or minor trauma and iatrogenic causes such as ones resulting from spinal puncture performed for diagnostic- or anesthetic-related purposes2,5). It can also occur spontaneously in patients with coagulation abnormalities, underlying neoplasm, or arteriovenous malformation7). However, spontaneous cervical spinal SDHs occurring in the absence of these underlying conditions have been very rarely reported11,12). Here we report a case of spontaneous non-traumatic acute SDH with normal hemostatic parameters presenting as neck pain and hemiparesis. Magnetic resonance images (MRI) was fully diagnostic and the patient was successfully treated with conservative management. We also present a discussion of the etiology, pathogenesis, and prognosis of this rare pathologic entity.
A 48-year-old woman with neck pain and motor weakness was referred to our emergency room. The patient's symptoms developed when she rose from her bed. The patient had no previous history of anticoagulant therapy or hematological coagulopathy, and was in good health before this episode. On physical examination, she was alert and fully oriented. No neurologic abnormalities were found in the cranial nerves and cerebellar system. However, sensory testing of right arm and leg demonstrated loss of touch along with pin-prick and vibration sensitivity. Motor examination revealed hemiparesis on right side (Grade III on arm and Grade I on leg).
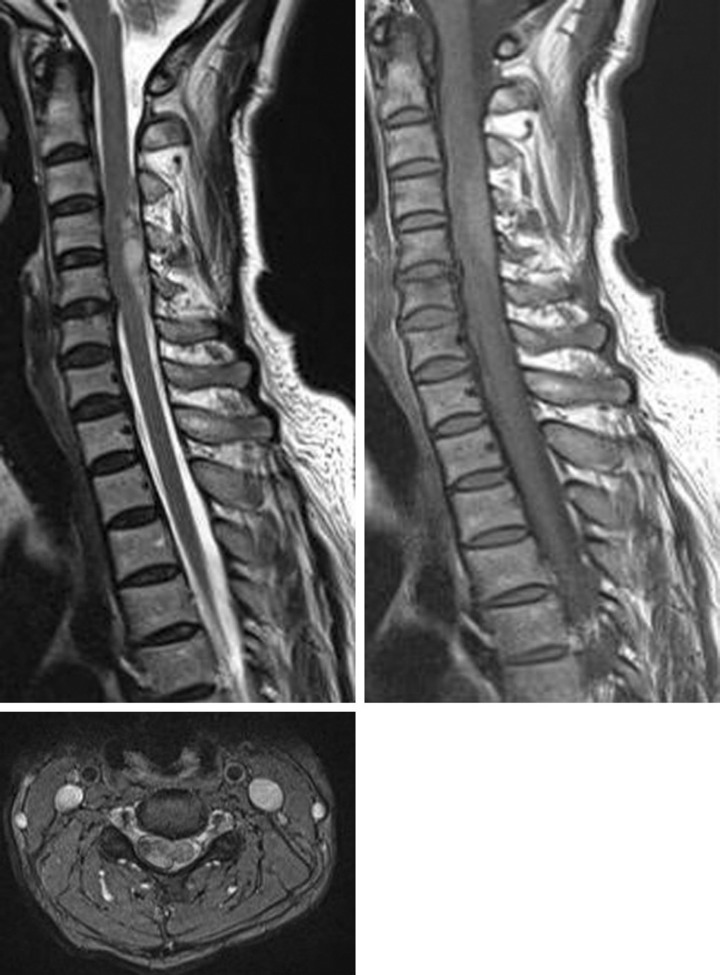
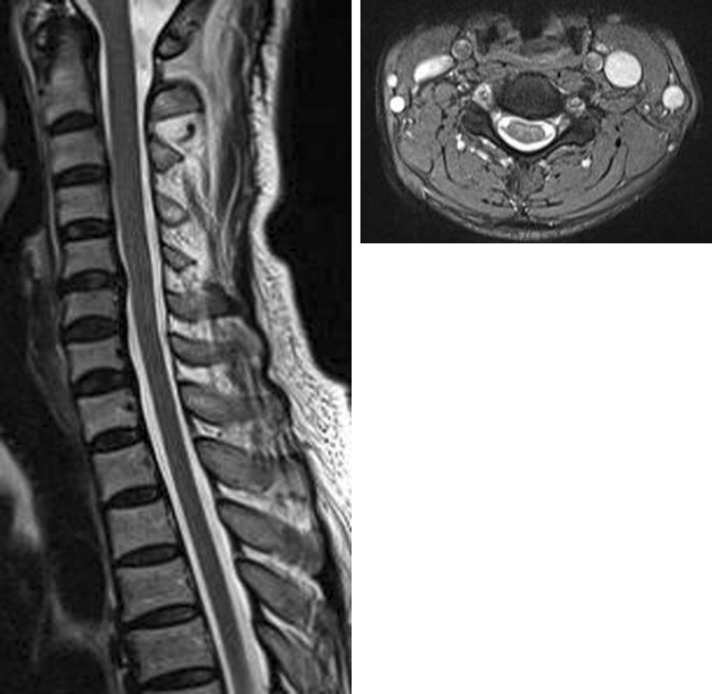
Brain computed tomography (CT) scans did not reveal any abnormal findings. The patient's coagulation profiles including platelet count, prothrombin time, and partial thromboplastin time were within normal ranges. Emergency MRI scan of the cervical spine was performed. The sagittal T1 and T2 weighted images revealed a dorsolateral subdural hematoma extending from C3 to C5 presenting as high signal in both sequences. The axial images showed left displacement of the spinal cord at this level (Fig. 1). The epidural fat was preserved, confirming the location of the hematoma. There was no signal void area, indicating that there were no abnormal vessels in the lesion. Based on these MR findings, the patient was diagnosed with an acute cervical spinal SDH in the right side at C3-C5 level. For differential diagnosis to distinguish this case from other conditions such as cervical epidural hematoma, a lumbar spinal puncture was performed. About 20CC of CSF was drained and cerebrospinal fluid (CSF) analysis revealed 190,000 red blood cells/mm3 and 267 white blood cells/mm3 (Fig. 2). An urgent laminectomy and hematoma removal was planned, but the patient's motor weakness gradually resolved during surgical preparation. At 5 hours after the symptom onset, her right side hemiparesis improved to Grade IV. The next day, her muscle power on the right side had fully recovered and she was able to walk without any assistance. MR images obtained 10 days after admission revealed that the spinal SDH had completely resolved (Fig. 3). The patient was in good health and free of neurological deficits during the 10 months follow-up period.
Acute spinal SDH is a rare pathological entity that is caused by compression of the spinal cord or cauda equina1). Although there is no evidence of any underlying causes and this type of hematoma appears spontaneously, several authors have reported that hematological disorders, anticoagulant therapy, spinal puncture, or traumatic brain injury predispose individuals to developing spinal SDH3,5). Acute spontaneous SDHs appearing in the absence these predisposing conditions are very rarely reported and are frequently located in the thoracic spine2). The spontaneous SDHs at cervical or cervicothoracic region are rare. Unlike the epidural space and intracranial anatomy of the dura, the spinal subdural space does not contain major blood vessels or bridging veins. Instead, the vasculature consists of only a delicate network of vessels that run along the lateral margins of the dura. Moreover, relatively larger and more vascularized epidural fatty tissues are present and the spinal dura does not adhere to bone. Thus, spinal epidural hematoma occurs more frequently than spinal SDH5).
The causes and origin of this type of hemorrhage in the subdrual space are still undefined. Rader et al.11) proposed that sudden and sharp increases in abdominal and thoracic pressure elevate intravascular pressure in the spinal subdural space to the extent that a momentary disparity between intravascular and extravascular pressure could result in the tearing of a spinal vessels. When cerebrospinal fluid (CSF) pressure is lower than intravascular pressure, vessels rupture and result in subarachnoid hemo- rrhage. The same sudden increases in pressure can cause rupturing of small extra-arachnoidal vessels located on the inner surface of the dura, resulting in a subdural hemo- rrhage. Several authors have described the presence of combined subdural and subarachnoid hemorrhages in patients9,13). This has led to the suggestion that subdural hemorrhage may originate in the more vascularized subarachnoid space and pass through the thin and delicate arachnoid membrane. Conversely, the hematoma can originate in the subdural space and then pass through the arachnoid membrane, giving rise to a concurrent subarachnoid hemorrhage. There are questions as to whether this small delicate network of vessels can be the source of hemorrhage4,8). In the present case, we couldn't confirm the presence of blood in both spaces because surgery was not performed. Although the degree of symptoms varies from mild motor-sensory deficit to serious sphincter deficits, spinal SDH can rapidly compromise the spinal cord or cauda equina and result in paralysis or acute deterioration with severe neurologic deficits. Therefore, prompt diagnosis and determining the extent of the hematoma are essential.
MRI is considered to be the best imaging technique for the diagnosis and follow-up of patients with spinal SDH6,10). This modality best depicts the extent of the hemorrhage and delineation from the epidural space. In commonly-used T2 weighted turbospinecho sequences, recently-developed hematomas are hyperintense to the spinal cord and iso-intense to CSF. In T1 weighted sequences, the blood is mostly iso-intense to the spinal cord and only slightly brighter than CSF. Alteration of the spinal cord is less conspicuous than in epidural hemorrhage because the distribution of the blood is semicircular with subsequent compression instead of displacement. The majority of hematomas are located ventral to the spinal cord or circumferentially with a major ventral part. However, it is difficult to differentiate between a subdural and epidural hematoma on the spine in some cases. In such instances, lumbar tapping is a useful diagnostic tool to determine the exact location of the hematoma5). It is widely accepted that prompt surgical evacuation should be performed before permanent irreversible damage to the spinal cord occurs when severe neurological symptoms or clinical worsening are observed. However, we did not perform emergency surgical decompression due to the early progressive improvement of the patient.
References
1. Boukobza M, Haddar D, Boissonet M, Merland JJ. Spinal subdural haematoma: a study of three cases. Clin Radiol 2001 56:475-480. PMID: 11428797.


2. Domenicucci M, Ramieri A, Ciappetta P, Delfini R. Nontraumatic acute spinal subdural hematoma: report of five cases and review of the literature. J Neurosurg 1999 91(1 Suppl):65-73. PMID: 10419371.


3. Hung KS, Lui CC, Wang CH, Wang CJ, Howng SL. Traumatic spinal subdural hematoma with spontaneous resolution. Spine (Phila Pa 1976) 2002 27:E534-E538. PMID: 12486364.


4. Kang HS, Chung CK, Kim HJ. Spontaneous spinal subdural hematoma with spontaneous resolution. Spinal Cord 2000 38:192-196. PMID: 10795940.


5. Kim HY, Ju CI, Kim SW. Acute cervical spinal subdural hematoma not related to head injury. J Korean Neurosurg Soc 2010 47:467-469. PMID: 20617096.



6. Küker W, Thiex R, Friese S, Freudenstein D, Reinges MH, Ernemann U, et al. Spinal subdural and epidural haematomas: diagnostic and therapeutic aspects in acute and subacute cases. Acta Neurochir (Wien) 2000 142:777-785. PMID: 10955672.


7. Kyriakides AE, Lalam RK, El Masry WS. Acute spontaneous spinal subdural hematoma presenting as paraplegia: a rare case. Spine (Phila Pa 1976) 2007 32:E619-E622. PMID: 17906565.


8. Longatti PL, Freschi P, Moro M, Trincia G, Carteri A. Spontaneous spinal subdural hematoma. J Neurosurg Sci 1994 38:197-199. PMID: 7782868.

9. Ma H, Kim IS. Idiopathic lumbosacral spinal chronic subdural hematoma. Korean J Spine 2012 9(1):41-43.



10. Post MJ, Becerra JL, Madsen PW, Puckett W, Quencer RM, Bunge RP, et al. Acute spinal subdural hematoma: MR and CT findings with pathologic correlates. AJNR Am J Neuroradiol 1994 15:1895-1905. PMID: 7863939.


11. RADER JP. Chronic subdural hematoma of the spinal cord: report of a case. N Engl J Med 1955 253:374-376. PMID: 13244833.


12. Reynolds AF Jr, Turner PT. Spinal subdural hematoma. Rocky Mt Med J 1978 75:199-200. PMID: 684338.

13. Schwartz FT, Sartawi MA, Fox JL. Unusual hematomas outside the spinal cord. Report of two cases. J Neurosurg 1973 39:249-251. PMID: 4719702.


14. Swann KW, Ropper AH, New PF, Poletti CE. Spontaneous spinal subarachnoid hemorrhage and subdural hematoma. Report of two cases. J Neurosurg 1984 61:975-980. PMID: 6491742.



- TOOLS
-
METRICS

-
- 5 Crossref
- Scopus
- 6,503 View
- 73 Download